Brazilian Woman Suffers Severe Skin Loss After Antidepressant Use
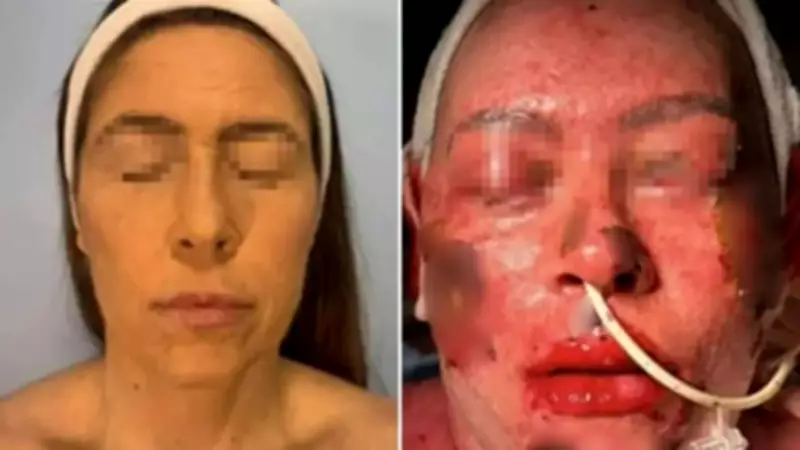
In a shocking medical case, a 42-year-old Brazilian woman experienced the loss of 55% of her skin following her use of a commonly prescribed antidepressant medication. The patient had been prescribed Lamotrigine, a drug frequently utilized for managing epilepsy and bipolar disorder, to help stabilize her mood. However, shortly after beginning the treatment, she noticed alarming symptoms as her skin started to blister and peel away dramatically.
Hospital Admission and Initial Misdiagnosis
Upon arrival at the hospital, the woman's condition was critical. Her entire face was described as raw, red, and actively bleeding. Significant skin loss was also evident on other areas of her body, including the neck, torso, pubic region, and several limbs. Initially, medical professionals suspected an acute bacterial infection and administered antibiotics. Further testing, however, revealed the presence of Pseudomonas aeruginosa bacteria, complicating her condition.
Specialists at the Hospital Beneficencia Portuguesa de São Paulo in Brazil ultimately diagnosed her with two severe, overlapping conditions: Stevens-Johnson syndrome (SJS) and toxic epidermal necrosis (TEN). These are rare but serious adverse reactions to medications that cause the skin to develop painful blisters and detach from the body.
The Critical Timeline and Symptoms
The patient's ordeal began two to three weeks prior to her hospital admission. She first developed lesions that progressively worsened, eventually necessitating urgent treatment in the Intensive Care Unit (ICU). In addition to the widespread blistering, she suffered from severe swelling across her entire body. Experts emphasize that a swift diagnosis and immediate management of the damaged skin are vital to prevent secondary infections, which can become life-threatening if left untreated, as noted in the Journal of Surgical Case Reports.
Innovative Treatment with Sheep Tissue Grafts
To address the extensive burns and promote healing, doctors employed an innovative treatment method. They applied grafts made from ovine forestomach matrix (OFM), which is derived from the stomach tissue of sheep, directly to the wounds on her face. This approach was chosen to accelerate the healing process.
Over a period of 17 days, the grafts were applied five times. Medical staff observed that the inflammation was markedly reduced following these applications. Encouraged by the success on her face, the same treatment was extended to the rest of her body. With frequent application, her skin showed visible improvements, becoming less inflamed and scarred.
Understanding Stevens-Johnson Syndrome
Stevens-Johnson Syndrome, previously known as Lyell Syndrome, and its more severe form, toxic epidermal necrolysis, are variants of the same rare, acute, and potentially fatal skin condition. Medications are responsible for triggering these reactions approximately 80% of the time.
According to the National Library of Medicine, the drugs most commonly associated with SJS/TEN include:
- Anticonvulsants like lamotrigine and phenytoin
- Allopurinol
- Various antibiotics
- Paracetamol (acetaminophen)
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
The NHS notes that such reactions are more likely to occur within the first eight weeks of starting a medication. Initial symptoms often include headaches, joint pain, and a cough, which are then followed by the development of a rash that escalates into severe blistering and skin detachment.