Understanding HPV and Its Direct Link to Cancer Development
Human Papillomavirus, commonly known as HPV, represents a group of over 200 related viruses, with certain high-risk strains directly implicated in the development of various cancers. Medical research has firmly established that persistent infection with these high-risk HPV types is the primary cause of cervical cancer, accounting for nearly all cases globally. Beyond cervical cancer, HPV is also linked to cancers of the anus, penis, vagina, vulva, and oropharynx (the back of the throat, including the base of the tongue and tonsils). The mechanism involves the virus integrating into the host's DNA, disrupting normal cell functions and leading to uncontrolled cell growth, which can progress to malignancy if left unchecked.
The Critical Role of Early Vaccination in Cancer Prevention
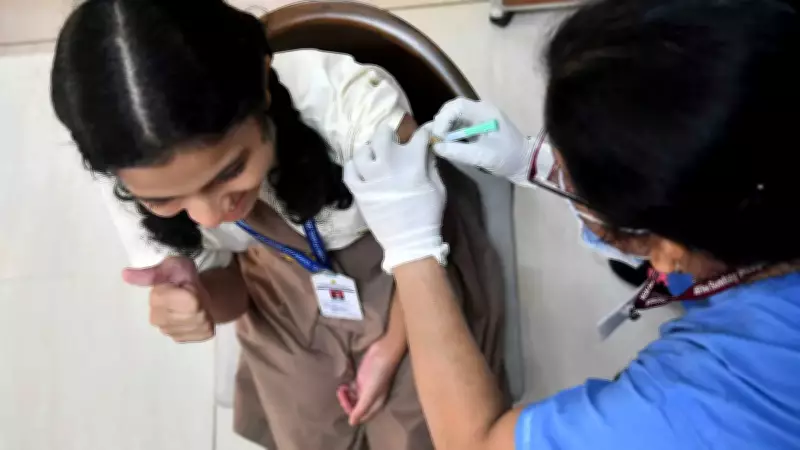
Vaccination against HPV is a powerful preventive tool, most effective when administered early, typically before exposure to the virus through sexual activity. The vaccines target the most common high-risk HPV strains, such as types 16 and 18, which are responsible for a significant majority of HPV-related cancers. By stimulating the immune system to produce antibodies, the vaccine provides protection against future infections, thereby reducing the risk of cancer development. Early vaccination, often recommended for adolescents around ages 11-12, offers the highest level of efficacy because it ensures immunity is established prior to potential viral exposure. This proactive approach not only safeguards individual health but also contributes to herd immunity, decreasing the overall prevalence of HPV in the population.
Expanding Awareness and Addressing Vaccination Barriers
Despite the proven benefits, HPV vaccination rates remain suboptimal in many regions due to factors like lack of awareness, misinformation, and cultural stigmas. Public health initiatives must focus on educating communities about the vaccine's safety and its role in preventing life-threatening cancers. Healthcare providers play a pivotal role in recommending the vaccine during routine check-ups, emphasizing its importance as part of comprehensive cancer prevention strategies. Additionally, addressing logistical challenges, such as vaccine accessibility and cost, is essential to ensure equitable protection across diverse populations. By overcoming these barriers, we can move closer to the global goal of eliminating HPV-related cancers through widespread immunization.
Long-Term Impact and Future Directions in HPV Management
The long-term impact of HPV vaccination is profound, with studies showing a significant reduction in precancerous lesions and cancer incidence in vaccinated populations. As vaccination programs expand, ongoing research continues to refine vaccine formulations and delivery methods, potentially broadening protection against additional HPV strains. Combining vaccination with regular screening, such as Pap tests and HPV DNA tests, forms a robust defense strategy, allowing for early detection and intervention when necessary. Ultimately, prioritizing early vaccination as a cornerstone of public health policy can lead to a substantial decline in cancer burdens, saving countless lives and reducing healthcare costs associated with cancer treatment.