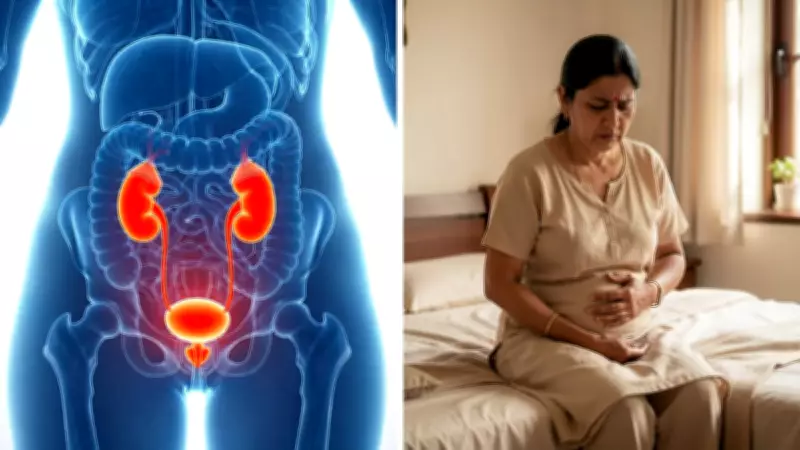
The Link Between Menopause and Increased UTI Risk
Urinary tract infections (UTIs) are a common health concern for women, but their incidence often sees a significant rise during the menopausal transition. This period, marked by the end of menstrual cycles, brings about profound physiological changes that directly impact urinary health. Understanding why UTIs become more frequent at this life stage is crucial for effective prevention and management.
Hormonal Shifts and Their Impact
The primary driver behind the increased susceptibility to UTIs during menopause is the decline in estrogen levels. Estrogen plays a vital role in maintaining the health of the urinary tract lining. It helps keep the tissues of the urethra and bladder resilient, moist, and rich in protective bacteria known as lactobacilli. As estrogen production decreases, these tissues can become thinner, drier, and more fragile—a condition often referred to as urogenital atrophy.
This thinning weakens the natural barrier against pathogens, making it easier for bacteria like Escherichia coli (E. coli) to adhere to and invade the urinary tract. Additionally, the reduction in lactobacilli alters the vaginal and urinary microbiome, reducing its ability to fend off harmful microbes. The result is a heightened vulnerability to infections that can lead to symptoms such as burning during urination, frequent urges to urinate, and pelvic discomfort.
Anatomical and Lifestyle Factors
Beyond hormonal changes, several other factors contribute to the rise in UTIs during menopause. The pelvic floor muscles may weaken over time, potentially leading to issues like urinary incontinence or incomplete bladder emptying. When urine remains in the bladder, it creates an environment conducive to bacterial growth. Changes in vaginal pH levels also occur, shifting from acidic to more alkaline, which further compromises the body's natural defenses against infection.
Lifestyle aspects can exacerbate these risks. For instance, decreased sexual activity or the use of certain hygiene products might influence urinary health. However, it's important to note that menopause itself is a key biological trigger, not merely a correlate of aging. Women in this phase should be particularly vigilant about symptoms and proactive in seeking medical advice to avoid complications like recurrent or kidney infections.
Prevention and Management Strategies
Addressing the increased risk of UTIs during menopause involves a combination of medical and lifestyle approaches. Healthcare providers often recommend:
- Topical Estrogen Therapy: Applied as creams, rings, or tablets, this can help restore the health of urinary and vaginal tissues, reducing infection risk.
- Hydration and Hygiene: Drinking plenty of water and practicing good urinary habits, such as wiping from front to back, can minimize bacterial exposure.
- Probiotics and Diet: Incorporating probiotics or cranberry products may support a healthy microbiome, though evidence varies.
- Regular Check-ups: Consulting a doctor for persistent symptoms ensures timely treatment, often with antibiotics tailored to menopausal needs.
By recognizing the multifaceted reasons behind the surge in UTIs during menopause, women can take empowered steps toward maintaining their urinary health. This knowledge not only aids in prevention but also fosters a better quality of life through informed healthcare decisions.